Dehiscence Dehiscence is defined as the separation of the sutured layers of the abdominal
wall and may be classified as partial or complete. In the case
of a partial dehiscence, one or more, but not all of the sutured layers
may separate. This situation may also be referred to as wound disruption. Complete
dehiscence is marked by separation of all layers resulting
in exposure of the peritoneal cavity. Synonyms include evisceration
and burst abdomen. The incidence of this complication has been quoted
as 0.3% to 3% of all pelvic surgeries, but it is currently thought
to occur in less than 1% of cases.33,34,35 Historically, the incidence was thought to be greater for vertical as
opposed to transverse incisions, but more recent studies have shown them
to be equal.35,36 ETIOLOGY AND PREVENTION. The main causes of dehiscence include failure of the suture to remain anchored
in the fascia, suture breakage, and knot failure. Of these, tissue
failure and improper suture choice are the most common.35,37 Since closure techniques involving permanent suture and wide bites of
tissue exist that effectively prevent dehiscence, the central problem
becomes one of recognizing the patient in whom the extra time taken to
use a more secure closure is justified. Risk factors for dehiscence are listed in Table 3. Inherent strength of abdominal wall tissue affects the risk of dehiscence
and, in turn, is also affected by such factors as age, sex, metabolic
disease, and the presence of malignancy. Patients over the age of 60 are
at increased risk, as are males with a ratio of 2.6 to 6.7: 1 over
females.36 Uremia and diabetes are associated with poor healing, as is vitamin C
deficiency in the malnourished patient. These underlying conditions should
be corrected if possible. White and co-workers found half of their
cases of burst abdomen occurred in patients with malignancy.38 The presence of these risk factors indicates the need for a closure that
is resistant to disruption such as a mass closure, Smead-Jones closure, or
placement of retention sutures. TABLE 3. Risk Factors for Dehiscence
Systemic factors Malnutrition
Hypoproteinemia
Chronic anemia
Vitamin C deficiency
Systemic steroids
Malignancy
Advanced age
Obesity
Infection
Previous radiation therapy
Chemotherapy
Increased stress on wound Chronic coughing
Ileus with GI distention
Ascites
Local wound factors Infection
Hematoma
Improper closure
Intraoperative technique Incision type
Suture type
Closure technique
Pressure necrosis
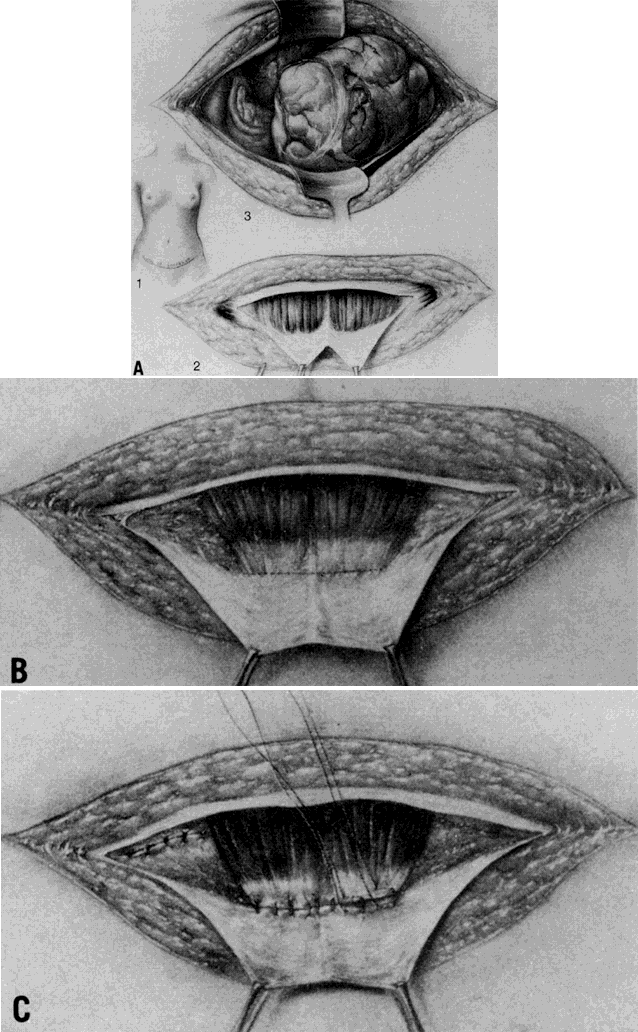
The method of closure plays an important part in wound security (Fig. 8). In layered closure each layer--peritoneum, fascia, subcutaneous tissue, and
skin--is closed separately, as opposed to mass closure where all
layers, usually excluding skin, are closed in a single unit. Ellis
cites mass closure as one of the most significant advances in reducing
the risk of burst abdomen. One of the key elements in mass closure is
the obligatory use of wide tissue bites (1.5–2 cm from the wound
edge) when placing the suture. Recall that the edge of the fascial incision
is often necrotic to some degree, resulting in tenuous tissue
strength and increased risk of disruption. if sutures are placed near
the cut edge. In a review, Wadstrom and Getdin27 found no studies proving an advantage to layered closure. Similar arguments
are forwarded in concluding that a continuous closure is superior
to interrupted sutures; no clinical advantage of interrupted closure
has been shown in the large majority of studies comparing the two. In
view of the :shorter operating time for continuous closure, it would
seem to be the obvious choice. Additionally, one could argue that it is
easier to tie two or three knots precisely than to tie precisely the
many knots required in interrupted closure. As noted above, to prevent
necrosis and subsequent wound disruption, sutures must not be placed
under undue tension. 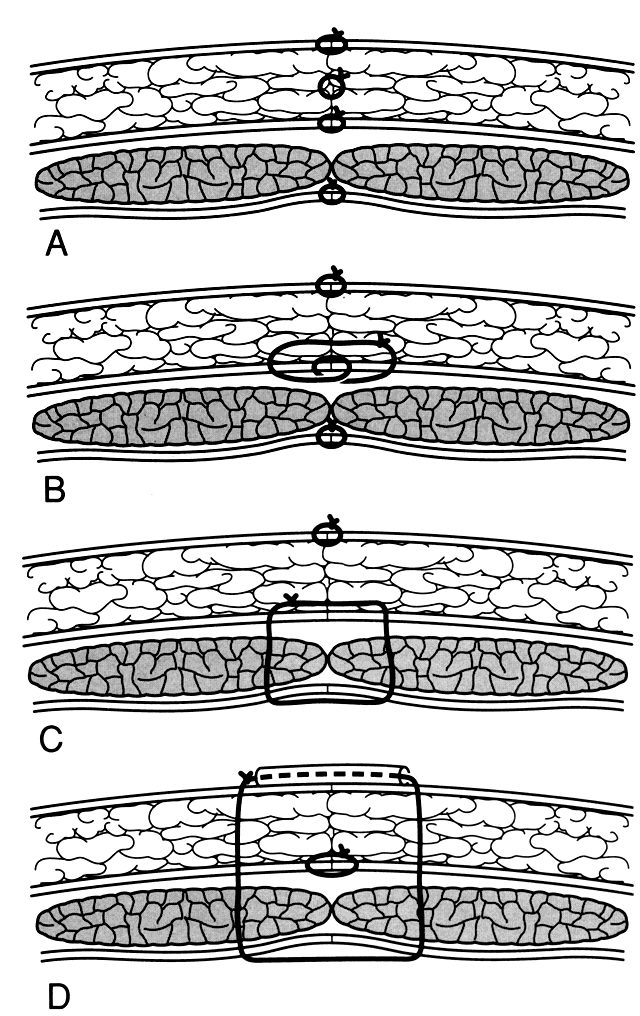 Fig. 8. Techniques of abdominal wall closure. A. Layered closure. B. Modified Smead-Jones closure. C. Mass closure. D. Retention suture. Fig. 8. Techniques of abdominal wall closure. A. Layered closure. B. Modified Smead-Jones closure. C. Mass closure. D. Retention suture.
|
In patients at unusually high risk of wound dehiscence, special consideration
should be given to using a closure that is, perhaps, somewhat more
time-consuming, but lessens the risk of disruption.39,40 When a wound dehiscence occurs, and permanent suture has been used, the
separation usually occurs where the sutures are inserted into the tissue. Therefore, unless
a weak or absorbable suture has been used, it
is usually not the suture that is at fault, but rather the way that the
sutures are anchored in the tissue.37 As previously mentioned, the further a suture is placed from the edge
of the wound, the more force is required to pull it out, making wide suture
placement a stronger technique. An additional factor that can be
used to increase the strength with which the suture can be anchored to
the tissue comes from distributing the tension that the suture places
on the tissue between at least two points. The Smead-Jones suture takes
advantage of this distribution by placing two bites on each side of
the wound edge in a far-near near-far arrangement as shown in Figure 8. Originally described, this technique was a mass closure that incorporated
both the muscle, fascia, and peritoneum of the abdominal wall. This
closure, incorporating all layers, is extremely strong, but it is usually
modified to have a separate peritoneal closure, with the Smead-Jones
stitches including only the musculofascial layer. This suture gains
its strength from the fact that before the suture can tear out of
the tissue, it would have to rupture the tissue at two points rather than
just one41 and can be done either as an interrupted technique or running suture. The most secure closure of the abdomen in-dudes both closure of the musculofascial
layers and placement of retention sutures through all layers
of the abdominal wall, including the skin and usually (although not
always) the peritoneum. It is virtually impossible for dehiscence to
occur while these sutures are in place because of the great amount of
tissue they would have to disrupt in order to pull out. They are usually
placed with a number 1, or greater, suture, and are especially useful
in treating a wound that has already undergone dehiscence. Proper suture selection will decrease the risk of dehiscence in patients
at normal risk. Clinical studies have shown that wound disruption is
most likely to occur in the early postoperative period, usually 5 to 8 days
after surgery. Both theoretical concerns about maintenance of suture
strength and clinical studies agree that there is no place for catgut
sutures in fascial closure. Other absorbable sutures, such as polyglycolic
acid (Dexon) and polyglactic acid (Vicryl), even losing up
to 80% of its tensile strength in 2 weeks,42 seem to compare favorably to permanent sutures, such as Prolene, in healthy
patients undergoing elective surgery who are at no unusual risk
for dehiscencefi As we will see below, there may be concern about the
more distant complication of wound hernia. In patients at risk for dehiscence, permanent
sutures are needed. In addition to the way in which a wound is closed, the stresses placed
upon it are important. Mechanical factors such as abdominal distension
from ileus, vomiting, and chronic cough may also play a role and should, therefore, be
treated when present or prevented when possible in the
patient already at risk due to other risk factors. Other factors that may weaken a wound include the presence of hematoma, wound
infection, and obesity. A hematoma will disrupt tissues, preventing
approximation as well as providing an excellent nidus for infection. More
often than not, wound dehiscence is associated with a combination
of events that, when recognized, calls for meticulous preoperative
preparation, wound closure, and postoperative care. DIAGNOSIS AND TREATMENT. Due to the increased morbidity and mortality associated with dehiscence, diagnosis
and treatment should be prompt. Mortality as high as 15% to 20% has
been reported in the literature, although more recent studies
demonstrate a rate around 10%. Mortality is not solely due to the dehiscence, however; these
patients are often ill with other chronic disease
and undergo a second anesthetic. Wound disruption usually occurs on the sixth to eighth postoperative day. Evisceration
will be apparent on simple inspection. When this is the
case, the intestines should be covered with a saline-moistened towel
and immediate steps taken to close the incision in the operating room. Although
lesser degrees of disruption may be asymptomatic, many patients
have a sense of something “giving way.” The most common
complaint is that of a profuse serosanguineous discharge from the wound. When
disruption is strongly suspected, careful exploration may best
be accomplished in the operating room with suitable anesthetic. In
any event, the wound should be opened as necessary to aid in diagnosis
and the fascial closure critically evaluated for disruption. A broad-spectrum
antibiotic should be started as soon as cultures have been obtained. Once the patient is in the operating room, the wound must be cleansed carefully
and thoroughly. Debridement of the subcutaneous tissue and fascia
should be accomplished as necessary. Strict attention must be paid
to closure--in this case to mass closure. Permanent material of suitable
size (number 1 or larger) should be used along with, possibly, retention
sutures, depending on the patient's general health and other
etiologic factors. Undue suture tension must be avoided to reduce
the possibility of necrosis, and bites at least 2 cm from the edge should
be used. Retention sutures may be left in place for 14 to 21 days. Underlying
conditions should, of course, be treated (e.g., an NG tube placed if ileus is present). When malnutrition is present or
develops, hyperalimentation should be considered and followed by careful
dietary support once oral alimentation is resumed. Wound Hernia Wound herniation is defined as an incomplete dehiscence in which the peritoneum, subcutaneous
tissue, and skin remain intact, but the muscle
or fascia do not. As opposed to dehiscence that occurs and is recognized
in the early postoperative period, wound herniation follows apparently
satisfactory healing only to present with an incisional defect at
a later date. Although it has been said that most such defects occur before 6 months
and nearly all before 1 year, several studies with longer
patient follow-up have found occurrences up to 5 years after the initial
operation. For low midline incisions, the most often quoted incidence
is about 1% in uncomplicated cases; after wound infection, the risk
rises to about 10% and, after repair of a dehiscence, to about 30%. Ellis
maintains that the reported low incidence of wound hernias is
due in part to the lack of prolonged follow-up in most studies. In a review
of their own patients for up to 5 years after operation in a group
free from hernia at 1 year, an additional 5.8% incidence was found.44 These defects range from the small and insignificant to the large and
unsightly. When the fascial defect is small, the risk of volvu-lus and
infarction of the hernial contents is increased, but still uncommon. ETIOLOGY AND PREVENTION. Late wound separation is more common in the lower abdomen because of increased
hydrostatic pressure and the lack of the posterior rectus sheath
below the arcuate line and, for vertical incisions, the greater lateral
forces provided by the bulkier oblique muscles inferiorly. The underlying
cause is inadequate healing of the fascial layer--perhaps more
related to degree than representing a true difference in etiology when
compared to dehiscence. Causes may include fascial necrosis from initial
excessive suture tension or, secondarily, from abdominal distension
associated with ileus, postoperative nausea and vomiting, or pulmonary
disease resulting in chronic cough. Necrosis may, in turn, be followed
by suture pull-through due to the inadequate tissue strength. These
causes of late wound separation can be largely eliminated by placing
wide tissue bites and by approximating the tissue without undue tension. Poor
tissue vitality is also the common factor in wound hernias
associated with wound infections and after repair of dehiscence. One element
in reducing the risk of wound infections would be selection of
a permanent monofilament suture. Another strong association is fascial
closure with catgut suture due to its inadequate continuation of strength
during the period critical to healing 45,46 DIAGNOSIS AND TREATMENT. Consideration should be given to the diagnosis of hernia when, with the
patient lying supine and legs raised, an incisional bulging is noted. The
hernia is often asymptomatic, although the patient may complain of
a bulging, or even note apparent peristalsis with resolution upon lying
down followed, in turn, by recurrence when standing. The bulge may
increase with a Valsalva maneuver. On examination the fascial defect
is often palpable. Because torsion and infarction are uncommon, colic, distension, nausea, and
vomiting are unusual symptoms, and repair is
usually elective. Small, asymptomatic hernias need not be repaired; those
that are symptomatic, large, or disfiguring deserve operation. The
principles of repair are: - Meticulous isolation of the hernia sac2. Wide exposure of the fascia3. Careful
closure, possibly with use of a graft in the case of very large
defects.
Usually, the old skin scar is excised followed by careful dissection of
the subcutaneous tissue until the hernia sac is encountered. Wide isolation
of the sac is continued until the fascial edges are encountered
and adequately undermined. The sac may then be opened, and attention
turned to any adhesions of peritoneum, bowel, or omentum that are carefully
separated until the hernia sac can be closed with a purse string
suture, and excess sac excised. This dissection can be confusing, with
apparent secondary hernia sacs formed by multiple bowel adhesions which, in
turn, must be separated until sufficient normal anatomy can be
restored to permit a safe closure. The next task is isolation of the
fascial edges and freshening of them if the size of the defect will allow
primary closure. Several satisfactory approaches may be used, including
Smead-Jones closure, mass closure, and overlapping of fascia (pants-and-vest
closure). Theoretical considerations would point to the selection
of a permanent monofilament suture. Appropriate selections would
include 0 or 1 Prolene, nylon, or other permanent sutures. Wire, although
important historically, has no advantages over the newer, nonreactive, monofilament
sutures. Large defects may need to be closed with the use of prosthetic mesh (e.g., Merselene, Marlex, Gortex) to bridge the hiatus where approximation of
the fascial edges is not possible or causes undue tension. Other indications
for the use of a graft would include repair of a recurrent hernia, grossly
attenuated tissues, and fascia that is too weak for adequate
repair. Most commonly, the graft is placed anterior to the peritoneum
and transversalis fascia, and posterior to the rectus muscles. The
material must be anchored to the posterior aspect of the recti “on
stretch” to prevent folding when the muscles are approximated
in the midline. The anterior rectus sheath is approximated as closely
as possible. In some instances, dissection between the hernial sac and
the fascia may prove exceedingly difficult or impossible, in which
case the Marlex mesh may be anchored to the anterior aspect of the rectus
muscles and, again, the anterior rectus sheath would be approximated
as closely as possible. This location of the dissection is not as satisfactory, however, in
that the already increased risk of wound infection
due to the presertce of the graft is further increased by its proximity
to subcutaneous tissue and skin. Postoperatively, predisposing conditions for wound failure should be addressed
fastidiously, including control of nausea and vomiting, aggressive
and early treatment of ileus and pulmonary complications, and attention
to adequate nutrition. Wound Infection Wound infection has been reported to occur in 2% to 4% of all clean abdominal
incisions and up to 35% of all grossly contaminated incisions. Clean
incisions are defined as those initiated on prepared skin without
entering a contaminated viscus or encountering infection. Clean contaminated
wounds are the same as clean incisions, but a contaminated viscus, such
as the vagina that has been prepared, is entered without gross
spillage. A wound is classified as contaminated if an infected genitourinary
tract is entered or gross gastrointestinal spillage occurs. A
dirty wound is one that occurs when pus from an abscess is spilled
intraoperatively, or previously ruptured bowel is present. The rate of
infection varies not only according to increasing severity, but also
according to patient socioeconomic status, surgical technique, operating
time, obesity, age, and sex. ETIOLOGY AND PREVENTION. Infection is often initiated by direct inoculum of bacteria into the wound
from the patient's or surgeon's skin and is potentiated
by the presence of necrotic tissue. Proper preparation of both is necessary
to ensure the lowest possible rate of infection. If hair removal
is required, clipping immediately before surgery is preferable to shaving, and
either is preferable to shaving the evening before, which has
been associated with higher rates of wound infection. For the surgeon's
scrub, both initial antisepsis and the use of a long-acting antibacterial
agent is recommended; 20% to 40% of all gloves are punctured
during the course of an average operation 47 Although not currently the most popular choice, an initial scrub followed
by a 1-minute application of alcohol in an emollient base or the chlorhexidine
gluconate-alcohol hand rinse (Hibistat) would represent the
best possible preparation. After adequate skin antisepsis, multiple
intraoperative factors come to bear. Since devitalized tissue offers increased opportunity for poor wound healing
and infection, every effort should be made to minimize infection's
presence, including meticulous incisional technique with a stainless
steel scalpel and precise hemostasis with cautery or fine, nonreactive
suture. These same considerations hold true while operating (i.e., creation of the smallest possible pericles, only precise use of the electrocautery, avoidance
of ischemic closure of the vaginal cuff). Mass
closure of the abdominal wall with continuous mortoff-lament suture would
seem preferable in theory, although clinical studies have not yet
supported this view (other considerations, such as decreased risk of
dehiscence, may suggest this combination).27 Other closure considerations include copious irrigation with nonirritating
physiologic solutions, especially in wounds other than those classified
as clean. Even in clean wounds, however, irrigation removes fragments
of free tissue and fat globules from separated adipose cells that
will prolong inflammation and delay repair. Drains may be placed in
the subcutaneous tissue when diffuse oozing resistant to hemostatic efforts
is present. Soft drains, such as the Penrose, have been replaced
by closed suction drains brought out through a separate stab wound with
improved results (i.e., decreased rates of infection and hematoma). A trial of closed, subcutaneous
drains alternately placed in suction and irrigated every 8 hours
for 3 days with an antibiotic solution showed possible benefit in grossly
infected wounds, but probably are not justified in clean contaminated
wounds.48 A more traditional and proven approach to the contaminated wound is delayed
primary closure, either closed in delayed primary fashion or allowed
to heal by secondary intention. With delayed primary closure, Verrier
and colleagues showed a decrease in infection rates in contaminated
wounds from 11.1% to 4.8% and in infected wounds from 33% to 6.6%.49 Primary closure of the skin and subcutaneous tissues is defined as closure
at the time of the initial operation, and secondary closure indicates
closure after granulation tissue has formed either with suturing or
spontaneously as healing by secondary intention. A delayed primary closure
is one in which the subcutaneous tissue and skin are not closed
at the time of initial surgery, but covered by a :sterile dressing and
then closed some days later (usually on the fourth day), but before
the formation of granulation tissue. Sutures can be placed during the
original operation and left to be tied later, or the wound can be sutured
under local anesthesia in the patient's room. During this time, the
body's immune response has had a chance to clean the wound, and
microscopic capillary formation has begun, creating excellent oxygenation
of the wound edge. Closure of the wound on the fourth day greatly
decreases the chance of infection, allowing patients to avoid the
potentially serious problem of sepsis associated with wound infection. This
approach is most helpful during treatment of pelvic infection, especially
in patients with poor healing characteristics. In these patients, delayed
primary closure has resulted in an extremely low complication
rate. 50,51 DIAGNOSIS AND TREATMENT. Wound infections may present in several ways, depending on the extent of
the infection, host resistance, and the etiologic microorganisms. Early, mild
infections may be associated with only scant exudate from the
incision and, upon exploration of the wound, poor healing. Hemolytic
streptococcal organisms may cause erysipelas, an infection marked by
a rapidly extending erythematous cutaneous border. Deeper infections may
be found during the process of evaluation for postoperative fever and
may additionally be associated with erythema, induration of skin and
subcutaneous tissues or, possibly, fluctuation. One must be alert for
the rare but devastating signs of necrotizing infections, including
brawny edema, cutaneous sensory loss, and obvious necrosis. Patients with
necrotizing fasciitis need prompt and aggressive debridement under
general anesthesia to avoid death. In cases of contaminated and infected wounds, consideration should be given
to delayed primary or secondary closure. In these situations characteristics
of each case should be taken into account, such as the amount
of infected tissue left behind, nutritional status of the patient, presence
of diabetes, malignancy, or obesity--factors associated with
poor wound-healing. When the decision is made to proceed with delayed
closure, retention sutures may be placed. Permanent, monofilament suture
would be the best choice. Cultures, of course, should be obtained. Postoperatively, the
incision can be left covered until the fourth day, at
which time the attending physician assesses whether the wound is
clean enough to close. If there is any infected or necrotic tissue, then
regular dressing changes and debridement can be commenced postoperatively
until the wound is ready to close. Delayed primary closure may
be done using one of several techniques: closure with sutures placed, but
not tied, in the operating room; placement of sutures with local
anesthesia; or application of sterile adhesive strips. In the high-risk
patient, when coaptation of the wound is difficult, or if the wound
does not appear clean in a reasonable period of time, the wound may be
allowed to heal by secondary intention. Perhaps surprisingly, the cosmetic
result in such a case is equal to that of delayed primary closure. Careful
instruction prior to discharge and follow-up by a visiting
nurse will be very helpful to the patient and her family. Treatment for superficial and minor infections may consist only of application
of moist heat. Erysipelas usually responds rapidly to such local
treatment with the addition of penicillin. When discharge from the
wound is prominent, or fluctuation is thought to be present, the wound
should be explored and all areas presenting little resistance to separation
opened fully. Cultures should be obtained, appropriate antibiotics
should be started and the wound should be debrided and packed. Secondary
closure may be desirable and possible if the wound reveals healthy
granulation tissue 3 to 5 days after opening. Again, the patient may
be sent home with follow-up by a visiting nurse. Nerve Injury Nerve injury associated with abdominal incision can pose a distressing, and
often unexpected ending to an otherwise successful operation. Two
types of injury occur. First, the incision and closure may transect or
damage the nerves of the abdominal wall. Second, a retractor used during
the operation can cause injury to nerves on the posterior body wall. The most serious nerve damage is that to the fiemoral nerve, because of
the loss of innervation to the quadriceps muscle in the leg and loss
of the ability to extent the leg at the knee joint. This damage is usually
caused by the blades of a self-retaining retractor. The lateral blades
of these instruments can press upon the nerve as it emerges from
the lateral border of the psoas muscle before passing under the inguinal
ligament (Fig. 9). The frequency of femoral neuropathy after gynecologic surgery is surprisingly
common, occurring in approximately 10% of pelvic laparotomies.52,53,54 Fortunately, most of these cases resolve spontaneously, yet when a case
does not, it poses a significant problem. Damage to the nerve should
be suspected with loss of sensation in the anteromedial thigh, diminished
knee jerk, and weakness of extension of the knee, which creates a
specific problem climbing stairs. 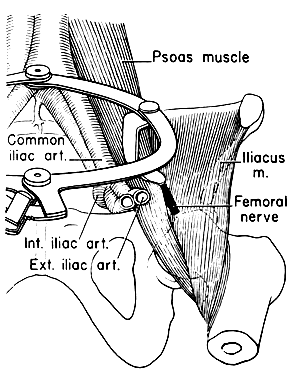 Fig. 9. Retractor inductor nerve injury.(Vosburg LF, Finn WF: Fernoral nerve impairment subsequent to hysterectomy. Am
J Obstet Gynecol 82: 931, 1961) Fig. 9. Retractor inductor nerve injury.(Vosburg LF, Finn WF: Fernoral nerve impairment subsequent to hysterectomy. Am
J Obstet Gynecol 82: 931, 1961)
|
In addition to damage to the main femoral nerve, retractor blades can compress
the genito-femoral nerve that emerges from the body of the psoas
muscle to lie on its muscle-belly. Although this situation creates
no motor abnormality, the loss of sensation in the upper medial thigh
and labium majus can be quite distressing. The risk of these complications is higher in thin individuals and when
retractors with deep blades have been used. Simply placing a laparotomy
pack over the retractor blades will not diminish the amount of force
that impinges on the nerve, and a space between the blade and nerve should
always be confirmed, remembering that some downward pressure will
unavoidably be placed on the retractor during surgery. Although the
nerve itself can not readily be palpated in the operating room, the psoas
muscle can be. It lies lateral to the external iliac artery, and identification
of the vessel by its pulse will lead the examining finger
laterally to the muscle. An additional type of injury that can occur is entrapment of the iliohypogastric
or ilioinguinal nerves in the lateral closure of a transverse
incision (Fig. 10)55 Transection of the nerve can lead to an area of anesthesia in the distribution
of the damaged nerve, and trapping them in a suture can give
rise to pain in the lower abdomen or groin. These nerves lie medial to
the anterior superior iliac spine, first, between the layers of the transversus
abdominus and internal oblique muscles, and then, more medially, come
to lie between the internal oblique and external oblique. Although
most surgeons fail to notice them during the lateral extension
of a transverse incision, they are sometimes visible in the lateral aspects
of the wound and should be looked for and avoided when seen. 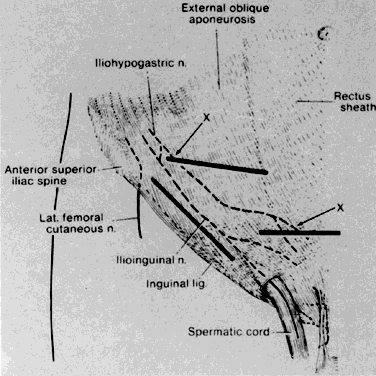 Fig. 10. Location of the iliohypogastric and ilioinguinal nerves that can be injured
during transverse abdominal incisions, as well as incisions in the
groin.(Skandalakis JE, Gray SW, Rowe JS: Anatomical Complications in General
Surgery. New York, McGraw-Hill, 1983) Fig. 10. Location of the iliohypogastric and ilioinguinal nerves that can be injured
during transverse abdominal incisions, as well as incisions in the
groin.(Skandalakis JE, Gray SW, Rowe JS: Anatomical Complications in General
Surgery. New York, McGraw-Hill, 1983)
|
Minor sensory abnormalities can arise when the nerve that innervates the
abdominal skin and that accompanies the blood vessels that run between
the rectus muscle and its sheath to reach the skin is transected during
elevation of the fascia off of the muscle in a Pfannenstiel incision. Because
of the extensive overlap of dermatomes here, this transection
is usually not a problem, but can cause troublesome loss of sensation
above the incision. |